Gender Affirming Mastectomy
Unfortunately, the average wait for gender affirming mastectomy in the NHS can be over 4 years. 2 years to be seen by a specialist, then another 2 years for surgery. Tragically, 25% of transgender or nonbinary people have struggled with severe mental health impacts.
The Harley Medical Group aims to be the leading provider of this service in the UK, with top quality care as a priority for all patients. Every patient is treated with dignity and respect throughout their journey*.
About Bilateral Mastectomy
This is a surgical procedure where the breast tissue, excluding the nipple and areolar, is removed, in a female to male transgender individual. There are various techniques utilised in masculinisation surgery, including:
- Double incision with or without free nipple graft
- Periareolar Incision (also called ‘keyhole’ or ‘concentric circumareolar’)
- Dermal flap technique
Something our patients worry about is the use of drains post-surgery, rest assured it is very unlikely that we will use drains in your surgery at The Harley Medical Group. This will not affect your result or the potentiality of any complications.
Surgery can last anywhere from 90 to 150 minutes depending on whether single surgeon or dual surgeon operating, size of chest and the technique used.
Mastectomy Techniques
Double Incision and free nipple graft
Can be done on any chest and is a good option to allow you choice of scar and nipple positioning
This approach involves removal of the excess skin, chest tissue and nipple via two incisions placed across either side of the chest to create two flaps. The chest tissue can then be removed and the flaps approximated and closed to achieve altered, masculinised contours. The nipple can then be prepared for reattachment and stitched into place.
In 30% of cases, nipple sensation is partially preserved but largely the nipples will be numb after surgery. Due to the nipple reconstruction process, there is a risk that nipple grafts may appear flattened post-operatively.
Periareolar Technique (Keyhole or concentric circumareolar)
Suitable for those with a small amount of chest tissue and little to no skin laxity.This technique creates very good male contours with minimal scarring and good nipple sensation. It is performed by making one circular incision around the border of your nipple, then a larger incision around that. Removing the breast tissue through this ring, then resizing and reattaching the areola by bringing together the edges of the larger incision. The nipple can be resized if wished, although this will impact nipple sensation.
Dermal Flap Technique
This is suitable for a medium to large-sized chest and is best suited to a person for whom keeping nipple sensation is very important.
In 70% of cases, nipple sensation is preserved as the nipple is left attached to the nerve supply on a piece of tissue which gets tucked under the skin of the chest. Although the areola (the coloured skin around the nipple) can be reduced with this technique, it is not recommended for the nipple itself to be reduced as this commonly reduces the nipple sensation.
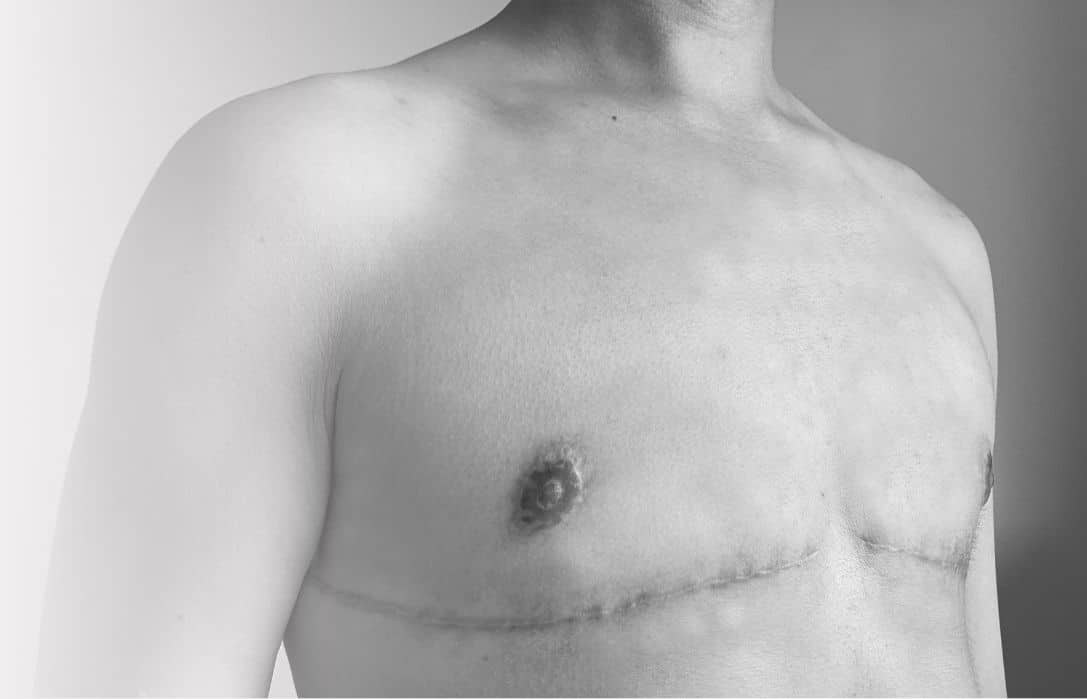
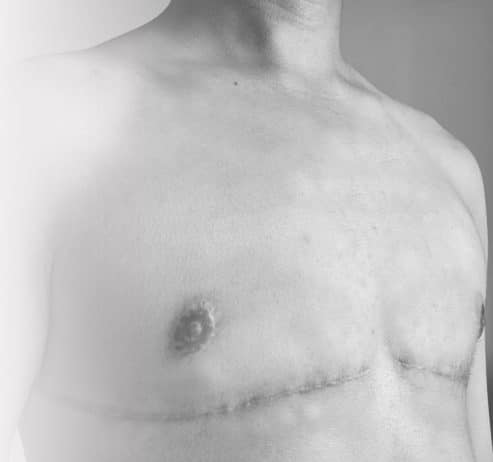
Scarring
Our surgeons will discuss with you how you hope your scars to be placed. They often recommend for the Incisions to be placed horizontally, below where the pectoral muscles are positioned, in a deliberately straight line to echo the shape of the pectoral muscles.
A tick shape can be created at the end of the incision towards the armpit which smooths out the contours and reduces the risk of ‘dog ears’ (protruding tissue from the outer part of the incision). Depending on the shape of a person’s chest, and their preferences, the surgeon may recommend for the scars to be joined in the middle in an inverted ‘v’ shape. Nipple positioning and size will be guided by your preference. You may choose to avoid reconstruction and reattachment, opting for tattooing instead. You have full ownership of what your chest will look like.
We can recommend a range of products to reduce the risk of scarring. However, we also know that many patients prefer to wear their scars with pride.
Patient journey
Each surgery is completely tailored to the desires and needs of each individual patient, there is no ‘one size fits all’ approach to gender affirmation surgery with The Harley Medical Group. Whether you want a typically masculine look, an androgynous look, or somewhere inbetween, our surgeons will work with you to understand the best look for you, down to the specifics of your nipple placement and size.
Treatment journey:
- Initial consultation with a Patient Advisor to discuss and assess your suitability and provide you with more information.
- Before your virtual consultation with your Surgeon, you will need information from your Gender Identity Clinic prior to this, which will then be reviewed by the surgeon before a decision is made to proceed or not.
- Initial video consultation with a surgeon - this allows for a more comfortable first meeting in the privacy of your own home. We want you to have a close relationship with your surgeon from the first instance. Please note it is helpful to the consultation if you can show the surgeon your chest for a few seconds during this session. However, your surgeon will completely understand if you are not comfortable with this and will work around it by asking you questions to describe your chest.
- Cooling off period of 2 weeks to allow you time to make your final decision.
- Your Patient Information Guide will be sent with everything you need to know after your first consultation. This allows you to think of any additional questions to bring with you to your first face-to-face consultation.
- Face-to-face consultation with your surgeon.
- Surgery can be scheduled at a convenient and available date.

Top surgery recovery and aftercare
Postoperative care and follow-up after surgical treatments for gender dysphoria are associated with good surgical and psychosocial outcomes (Monstrey et al., 2009).
The majority of procedures can be completed as a day case and you will be able to return home on the day of surgery. If you are not based in the Manchester area, you will need to stay in a local hotel for 2 nights with a trusted adult with you for support.
- We recommend you take 2-3 weeks off work from a desk-based job and 4-6 weeks off from a physically demanding job, post-surgery.
- No driving for 2 weeks.
- You must wear a compression garment for 2 weeks after your surgery, 22 out of 24 hours a day. Only take it off to wash the garment or to wash yourself. You may wish to have a second garment to rotate.
- Limit your arm movement and keep your elbows below the shoulders for six weeks after surgery.
- Sleep in an elevated position with your arms beside you, this is because your arms can naturally raise if you sleep on your front or side.
- Your dressings must stay untouched and dry for up to 10 days post-op when they will be removed at your local The Harley Medical Group clinic.
Your first post-operative appointment will be with a Nurse in the clinic approximately 10 days after your surgery.
6-8 weeks after your operation you will meet your Surgeon for a face-to-face post-op consultation to check your wound healing. A follow-up consultation can be arranged for 6 months’ time, which can take place virtually, if preferred. Please note you can ask for a review with a Nurse or Surgeon at any time should you have any concerns.
Testimonials
Verified review by an NHS patient at The Pines Hospital
Verified review by an NHS patient at The Pines Hospital
How much is a bilateral mastectomy?
Discover flexible payment options tailored to your budget and make your desired cosmetic procedure a reality. At The Harley Medical Group, we provide a wide range of cosmetic procedures, including top surgery. Our experienced consultants will carefully assess your goals and recommend the most suitable procedure to meet your expectations.
Rest assured that the price quoted during your consultation covers everything, including the procedure itself, overnight accommodations, and follow-up appointments. We believe in transparency, and there are no hidden costs involved.
To ensure affordability, we offer various monthly payment plans, including a 12-month 0% finance option for all procedures (minimum deposit of £500 required). Our patient advisors will gladly guide you through the available payment options specific to your recommended procedure.
Mastectomy prices
| Procedure | Guide Price (From) | Repayments Illustration 12 Months |
Repayments Illustration 60 Monthly |
Payment Calculator |
|---|---|---|---|---|
| Mastectomy | £8995 | £707.92pm | £197.53pm |
Choosing a surgeon
Make sure that you choose a surgeon who specialises in gender affirming care, and who works with you to understand the best outcome for you. The wider group of people involved in your care will also be equipped to deal with your needs, including the Hospital operating theatre teams and Patient Advisors.
Ask for recommendations within the community, read reviews online, and focus on patient outcomes that fit your desired look.
Meet our surgeons
Frequently Asked Questions
*
i. 41% of trans men reporting a past suicide attempt.
Suicide risk among transgender individuals
Shira Maguen &Jillian C. Shipherd
Pages 34-43 | Received 17 Jun 2009, Accepted 18 Dec 2009, Published online: 25 Mar 2010
ii. Depression is four times more common in Trans and gender diverse people than cis-gender populations
iii. Levels of depression in transgender people and its predictors: Results of a large matched control study with transgender people accessing clinical services. Author links open overlay panel, Gemma L. Witcomb a, Walter Pierre Bouman b, Laurence Claes c d, Nicola Brewin b, John R. Crawford e, Jon Arcelus b f.Journal of Affective Disorders, Volume 235, 1 August 2018, Pages 308-315