Top Surgery
Top Surgery is a procedure that is appropriate for transgender and nonbinary patients who are looking to achieve gender affirmation through surgical transition. There is no requirement to have completed a societal transition; for example changing your dress or pronouns, or a medical transition with hormone therapy, prior to a surgical procedure as gender affirming care means something different to each individual.
Requirements for those looking to have this procedure must:
- Be over 18
- Have a recommendation for top surgery from a gender specialist in a UK-based gender identity clinic
- BMI of between 18-32 and in general good health
- General good health and at a maintainable and stable weight
- Must stop smoking for a minimum of 4 weeks before the procedure as this could impact healing. This includes any nicotine replacement therapy such as vaping, nicotine patches or gum etc.
- There may be other contraindications unrelated to your gender status which will be discussed at consultation.
Gender affirming care is proven to improve patient well-being in terms of body satisfaction and gender dysphoria-related mental health problems*.
Top Surgery Overview
Beauty is in the eye of the beholder and you and your surgeon will work together to ensure that all decision-making is shared. The procedure for top surgery is completely bespoke to the wishes of each individual. To help make your journey smooth, we encourage our patients to consider their goals and expectations regarding their post-surgical appearance.
It may be helpful to bring photos of what ‘ideal’ looks like to you, as this will assist you in communicating your vision. A discussion can then take place between you and our expert surgeons about how achievable your desired results are. What does your chest need to look like so you can become your true self?
Patient journey
Each surgery is completely tailored to the desires and needs of each individual patient, there is no ‘one size fits all’ approach to gender affirmation surgery with The Harley Medical Group. Whether you want a typically masculine look, an androgynous look, or somewhere inbetween, our surgeons will work with you to understand the best look for you, down to the specifics of your nipple placement and size.
Treatment journey:
- Initial consultation with a Patient Advisor to discuss and assess your suitability and provide you with more information.
- Before your virtual consultation with your Surgeon, you will need information from your Gender Identity Clinic prior to this, which will then be reviewed by the surgeon before a decision is made to proceed or not.
- Initial video consultation with a surgeon - this allows for a more comfortable first meeting in the privacy of your own home. We want you to have a close relationship with your surgeon from the first instance. Please note it is helpful to the consultation if you can show the surgeon your chest for a few seconds during this session. However, your surgeon will completely understand if you are not comfortable with this and will work around it by asking you questions to describe your chest.
- Cooling off period of 2 weeks to allow you time to make your final decision.
- Your Patient Information Guide will be sent with everything you need to know after your first consultation. This allows you to think of any additional questions to bring with you to your first face-to-face consultation.
- Face-to-face consultation with your surgeon.
- Surgery can be scheduled at a convenient and available date.
The procedures for Top Surgery

Gender Affirming Augmentation
Unsure?
Request a consultation
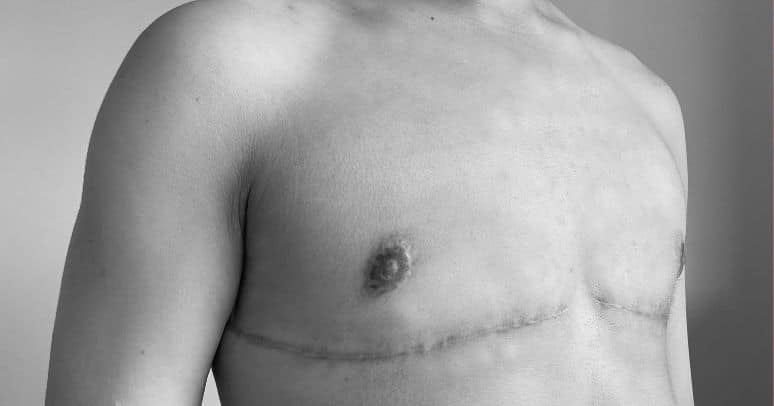
Mastectomy
The benefits of top surgery
In general, social and medical transition are both associated with a reduction in mental health problems.** A 2019 study found that following top surgery, measures of quality of life and sexual confidence improved significantly. 86% of participants reported an improvement in gender dysphoria-related mental health conditions.
Top surgery had major positive effects on all mental health and quality-of-life metrics, markedly improving the daily lives and function of transgender and non-binary in individuals who choose to undergo it.*** Strong evidence from years of research demonstrates the benefits in wellbeing of gender-affirming treatments, including surgical procedures.****
- Reduction in mental health problems
- Positive effect on quality-of-life
- Improved wellbeing
Top surgery recovery and aftercare
Postoperative care and follow-up after surgical treatments for gender dysphoria are associated with good surgical and psychosocial outcomes (Monstrey et al., 2009).
The majority of procedures can be completed as a day case and you will be able to return home on the day of surgery. If you are not based in the Manchester area, you will need to stay in a local hotel for 2 nights with a trusted adult with you for support.
- We recommend you take 2-3 weeks off work from a desk-based job and 4-6 weeks off from a physically demanding job, post-surgery.
- No driving for 2 weeks.
- You must wear a compression garment for 2 weeks after your surgery, 22 out of 24 hours a day. Only take it off to wash the garment or to wash yourself. You may wish to have a second garment to rotate.
- Limit your arm movement and keep your elbows below the shoulders for six weeks after surgery.
- Sleep in an elevated position with your arms beside you, this is because your arms can naturally raise if you sleep on your front or side.
- Your dressings must stay untouched and dry for up to 10 days post-op when they will be removed at your local The Harley Medical Group clinic.
Your first post-operative appointment will be with a Nurse in the clinic approximately 10 days after your surgery.
6-8 weeks after your operation you will meet your Surgeon for a face-to-face post-op consultation to check your wound healing. A follow-up consultation can be arranged for 6 months’ time, which can take place virtually, if preferred. Please note you can ask for a review with a Nurse or Surgeon at any time should you have any concerns.
Testimonials
Verified review by an NHS patient at The Pines Hospital
Verified review by an NHS patient at
How much is a top surgery?
Discover flexible payment options tailored to your budget and make your desired cosmetic procedure a reality. At The Harley Medical Group, we provide a wide range of cosmetic procedures, including top surgery and gender-affirming augmentation. Our experienced consultants will carefully assess your goals and recommend the most suitable procedure to meet your expectations.
Rest assured that the price quoted during your consultation covers everything, including the procedure itself, overnight accommodations, and follow-up appointments. We believe in transparency, and there are no hidden costs involved.
To ensure affordability, we offer various monthly payment plans, including a 12-month 0% finance option for all procedures (minimum deposit of £500 required). Our patient advisors will gladly guide you through the available payment options specific to your recommended procedure.
Top surgery prices
| Procedure | Guide Price (From) | Repayments Illustration 12 Months |
Repayments Illustration 60 Monthly |
Payment Calculator |
|---|---|---|---|---|
| Top Surgery Breast Augmentation | £6995 | £582.92pm | £162.65pm | |
| Top Surgery Reduction | £7995 | £624.58pm | £174.28pm | |
| Mastectomy | £8995 | £707.92pm | £197.53pm |
Choosing a surgeon
Make sure that you choose a surgeon who specialises in gender affirming care, and who works with you to understand the best outcome for you. The wider group of people involved in your care will also be equipped to deal with your needs, including the Hospital operating theatre teams and Patient Advisors.
Ask for recommendations within the community, read reviews online, and focus on patient outcomes that fit your desired look.
Meet our surgeons
Frequently Asked Questions
*Park RH, Liu YT, Samuel A, Gurganus M, Gampper TJ, Corbett ST, Shahane A, Stranix JT. Long-term Outcomes After Gender-Affirming Surgery: 40-Year Follow-up Study. Ann Plast Surg. 2022 Oct 1;89(4):431-436. doi: 10.1097/SAP.0000000000003233. PMID: 36149983.
**WPATH SOC 8, Aldridge et al., 2020; Bouman et al., 2017; Durwood et al., 2017; Glynn et al., 2016; Hughto & Reisner, 2016; Wilson et al., 2015; Witcomb et al., 2018).
** Poudrier G, Nolan IT, Cook TE, Saia W, Motosko CC, Stranix JT, Thomson JE, Gothard MD, Hazen A. Assessing Quality of Life and Patient-Reported Satisfaction with Masculinizing Top Surgery: A Mixed-Methods Descriptive Survey Study. Plast Reconstr Surg. 2019 Jan;143(1):272-279. doi: 10.1097/PRS.0000000000005113. PMID: 30286047.
**** Aldridge et al., 2020; Heylens, Verroken et al., 2014; International Journal of Transgender Health S37 White Hughto & Reisner, 2016)




